Where We Work
See our interactive map

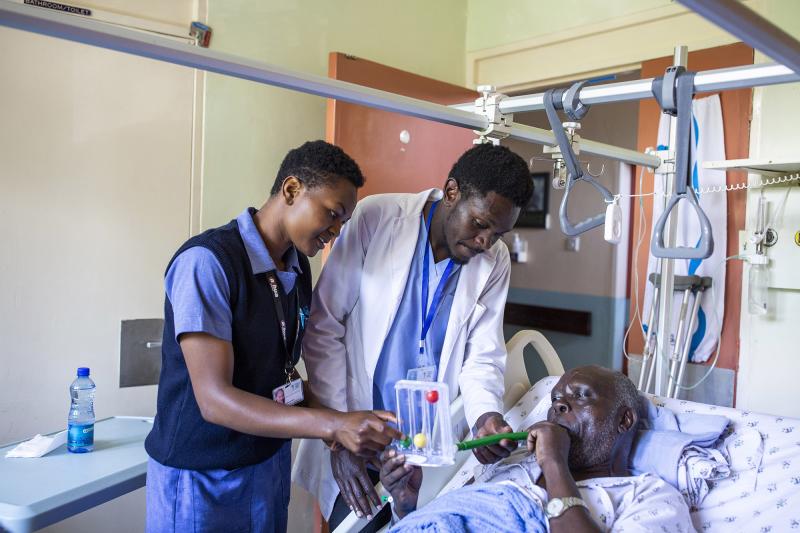
Nursing students Catherine Kimeu (left) and Samuel Kamau Kuria (center) care for a client in a health facility in Kenya. Like nurses all over the world, they face gender-related stereotypes and barriers at work. Those challenges keep many young people from pursuing much-needed nursing careers. Photo by Patrick Meinhardt for IntraHealth International.
Here's what we learned from young Kenyans about what gender inequality in nursing looks like for them.
What does gender inequality look like for nurses in Kenya? How does it affect nurses every day at work? And what does it mean for the country’s response to the COVID-19 pandemic?
We’ve found that young people are a key part of the answers to these questions. More than half of the world’s population is under 30, with an even higher proportion in sub-Saharan Africa.
Health systems are fighting the COVID-19 pandemic with only half their reserves if they don’t meaningfully engage young people in health workforce leadership, particularly nursing.
Young Kenyans are looking for careers where they can give back to their communities, but they often aren’t finding the support they need to enter health workforce professions. This is especially true for women, who make up 90% the nursing workforce worldwide but occupy only 25% of leadership roles.
The stereotype was that nursing is only for women because it “requires a big heart and compassionate mind.”
Here are some of the things we’ve learned from young Kenyans about what might help address these issues.
Despite increasing recognition of the gendered perceptions of health work (nursing and midwifery in particular), social changes to address these barriers are slow to come.
Nursing student Jane Muthoni Mutegi grew up believing the pervasive stereotype in her community that nursing is a job only for women because it “requires a big heart and compassionate mind.” Meanwhile, male nursing student Samuel Kamau Kuria’s decision to pursue nursing was met with negativity—his friends and family calling him a “coward.”
Another student, Catherine Kimeu, is scared that becoming pregnant will have a huge impact on her job. Unfortunately, she has reason to believe this -- when one of her colleagues was required to be on bedrest for 28 weeks due to a complicated pregnancy, she lost her job while also facing blame from her husband.
Rose Irungu, a fellow student, has also seen recent mothers forced to return to work after only three months (Kenya’s paid maternity leave time) even though the World Health Organization recommends six months of exclusive breastfeeding.
Kenyan health workers are routinely deployed far away from home, which makes many students concerned about whether and how they might raise their own families.

Catherine Kimeu. Photo by by Patrick Meinhardt for IntraHealth International.
There are also difficulties outside of the clinic. Jane has seen multiple female nurses struggle with their husbands not trusting them about being required to work overnight, and their communities often think of nursing jobs as low-skill, simply “cleaning wounds.”
When Samuel was growing up in rural Kenya, there were no doctors or nurses in his community. Today there are just two.
Despite the challenges they face on the job, many students want to return to their home communities once they finish schooling and work for those who supported them (including communities that fundraised for their school fees on their behalf).
This illustrates the benefits of a key intervention often overlooked in the health workforce: recruiting from the most underserved communities, thereby encouraging community trust and ownership of health outcomes.

Samuel Kamau Kuria. Photo by Patrick Meinhardt for IntraHealth International.
School fees continue to be prohibitive for many students in Kenya. Students are routinely sent home if they cannot come up with funding, which can derail their education entirely.
The Afya Elimu Fund, which provides loans to students for educational fees, is one way Kenya is addressing this. Students pay their loans back once they are employed, creating a cycle of support and adding to the pot of funds for the following year’s class.
Without job security in nursing, the shortage of health workers will only continue to grow.
Many young Kenyans are interested in pursuing nursing in part because of job security, as nurses are always needed and demand for their skillset is only increasing. However, contracts are often short-term, Samuel says.
“After that period, you have to renew your license or maybe your contract,” he says. “So your job is really not that permanent.”
If nursing can’t provide the job security necessary to draw in students who need to support themselves and their families, the shortage of health workers will only continue to grow.
Today, health workers everywhere face an extraordinary test in the form of a pandemic that has stretched health systems to their limits and brought the global economy to a halt. COVID-19 is a painful example of what happens when we neglect to invest in resilient health systems and the frontline health workers who keep them running.
As the first line of defense for global health security, health workers, particularly nurses, are needed to help prevent, detect, and respond to outbreaks like COVID-19 in their own communities.
Policies that support these critical professionals are needed to address the major challenges that prevent both women and men from effectively pursuing nursing careers. These include recruiting from local areas to develop community expertise, mitigating gender-related barriers, and adequately investing in training and continuous education to attract young people into this vital sector.
The negative perceptions of nurses and the barriers they face due to gender inequality and societal norms must be removed to make nursing a career that women are able to pursue and that men are encouraged to join to address critical gaps in frontline health workforce.
Without concrete policies that address the intersection of youth engagement and frontline health workforce, COVID-19 and future pandemics could continue to devastate countries around the world.
IntraHealth International’s Carol Bales and Samantha Rick interviewed nursing students and nurses in Kenya as part of a forthcoming case study on nursing leadership funded by Johnson and Johnson. Jane, Catherine, Rose, and Samuel are students at A.I.C. Kijabe College of Health Sciences in Kenya.
This post originally appeared on the Frontline Health Workers Coalition blog.
Get the latest updates from the blog and eNews




