Where We Work
See our interactive map

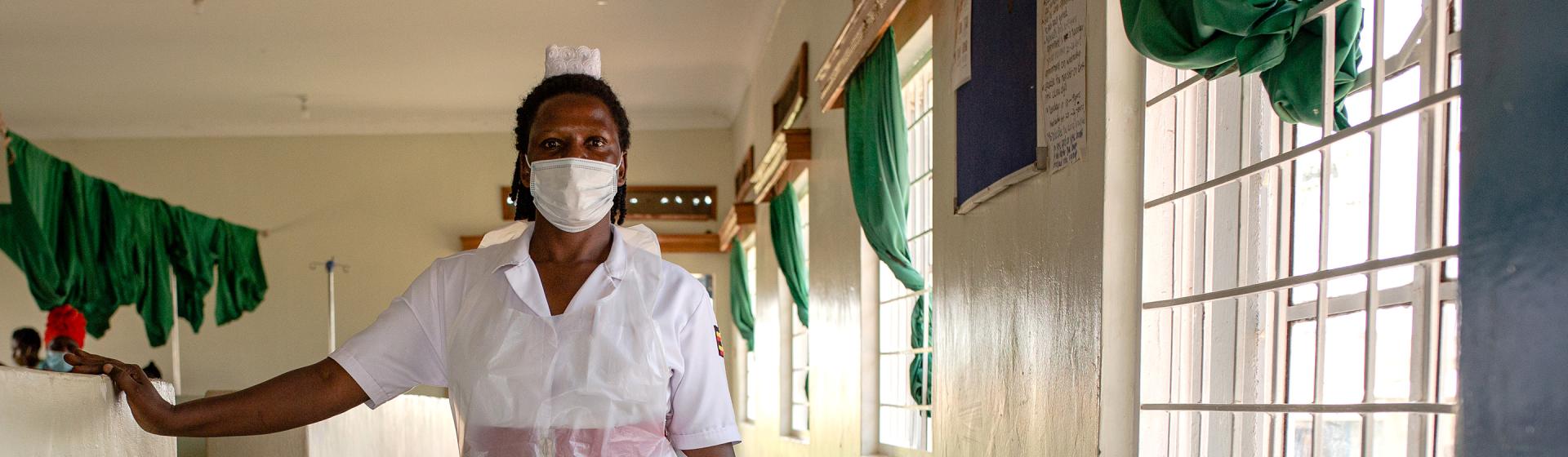

Polly Dunford, President & CEO of IntraHealth, visits Mbale Regional Referral Hospital in Uganda. Photo by Esther Ruth Mbabazi for IntraHealth International.
Strong data systems allow countries to surge health workers during emergencies. New funding should cover this.
US funding for global health security has surged in the last few years, and now Congress has just approved a $510 million increase for fiscal year 2022, nearly doubling current funding. President Biden is proposing even greater increases for fiscal year 2023 in his new budget proposal, including a multilateral fund for global health security and pandemic preparedness. The US has already pledged $250 million to this proposed fund, which has a goal of $10 billion in annual funding from the global community.
The urgent question is this: How do we best use these funds?
The difficulties many countries have faced in responding to COVID-19 and rapidly delivering vaccines, tests, treatment, and supportive care have shone a spotlight on vulnerabilities in health systems and workforces around the world.Historically, US global health security funding for the health workforce has focused on training field epidemiologists and preventing and detecting zoonotic diseases—valuable and necessary functions. The multilateral global health security agenda, which the US supports, has a similar emphasis for the workforce.
But high-level reviews of the lessons we’ve learned from COVID-19, such as the Independent Panel for Pandemic Preparedness and Response, have called for much broader investments in human resources to improve resilience.
We must expand our definition of global health security.
We must expand our definition of global health security to go beyond the traditional focus on disease surveillance capacity.
Frontline health workers—including community health workers—are every country's first defense when it comes to detecting, reporting, and responding to emerging threats and to building communities’ trust in their health systems. These workers need medical equipment, supplies, PPE, access to COVID-19 therapeutics, and solid, up-to-date data to do their jobs.So our definition of global health security must include them. We can start by adding investments in the information and communication systems health workers need to do their jobs—the same systems that allow governments to make the most of their limited workforces by allocating them as efficiently as possible during emergencies.
I hear this consistently from IntraHealth International’s program leaders around the world.
“Clinical health workers play a major role in public health,” says Janet Muriuki, a physician from Kenya and our senior director for health workforce development. “We need to teach health managers how to use data for informed decision-making. This includes systems that ensure real-time and up-to-date data. All of which calls for a human resource information system with dashboards that can answer questions based on national and subnational needs.”
These systems—and the level of data literacy Muriuki describes—are paramount to our global health security.
During any emergency, governments must be able to surge their health workers to outbreak zones, where they’re needed most. These surges require careful planning to minimize impact on other health services. And they require real-time information on the location and skillsets of health workers, including the community health workers who are invaluable in spreading the word and helping keep primary care available during emergencies.
But what if a government has no idea where the country’s health workers already are, whether they’re trained to deal with emerging infectious diseases, or even how to reach them? Unfortunately, this is the case for many countries right now. Current US government funding for global health security does not help ministries of health know where their health workers are, what skills they currently possess, what further capacity they need, or how to best deploy them.
That’s a big problem.
Fortunately, there are human resources information systems out there—like IntraHealth’s iHRIS, which is free and open source—that can give decision-makers the data they need to surge health workers as part of a rapid response to any emergency. In fact, we worked with officials in Mali and Kenya during the beginning of the pandemic to use iHRIS data as part of predicting COVID-19 hotspots and making sure health workers were available when and where they were needed most.
Combined with an interoperable communication system such as mHero, governments can use these systems to not only surge health workers, but to track vaccination status among health workers, generate reminders about follow-up doses, monitor health worker performance and service delivery data, and more.
By harnessing the full potential of their data through interoperable health information systems, health officials can strategically deploy health workers where they’re needed most before and during pandemics, humanitarian emergencies, and other emerging threats.Health workers are at the very heart of global health security.
“The agility with which countries were able to manage surge health workforce demands has been a key difference between successful and struggling responses,” the Independent Panel for Pandemic Preparedness and Response reported in their assessment of the COVID-19 response.
We should heed this assessment and recognize that health workers are at the very heart of global health security. When we envision a world prepared to respond to COVID-19 or the next pandemic, it must be one where governments have funding and personnel to keep them and their systems strong, keep their data up to date, and interpret them both every day and during emergencies.
On April 5, 9 a.m. ET, we'll talk about this and more during Health Workers Count for Global Health Security: Here’s Why. This virtual event during World Health Worker Week 2022 will feature experts from around the world, including:
Denis Ako-Arrey, chief of party, RHITES-E, IntraHealth International
Richard Greene, USAID lead on global health security agenda
Dr. Ahmed Ogwell Ouma, deputy director, Africa CDC
Margaret Odera, community health worker and mentor mother in Kenya
Moderator: Janet Muriuki, senior director of health workforce development, IntraHealth International
Want to get more stories like this delivered to your inbox? Sign up for our mailing list.
Get the latest updates from the blog and eNews




