Where We Work
See our interactive map

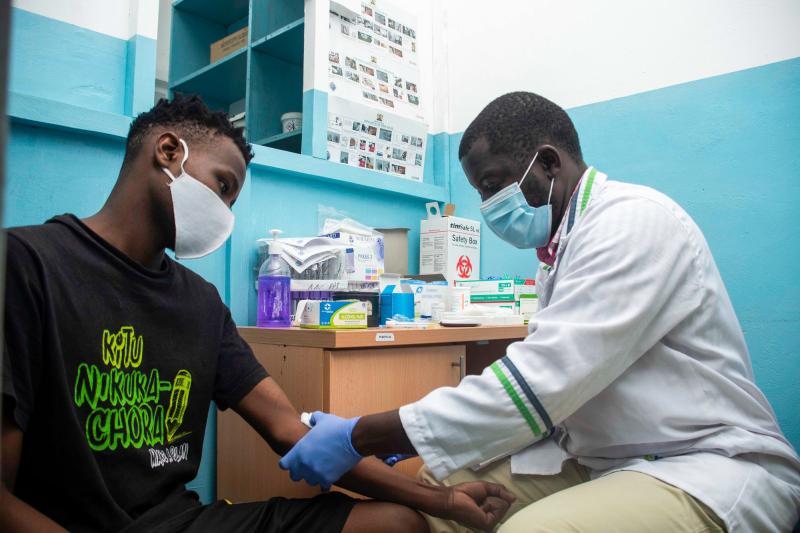
Nicodemas Ondies, medical lab officer, takes samples from a client at the Tudor Subcounty Hospital in Kenya. Photo by Edwin Joe for IntraHealth International.
A systems approach would improve the health and well-being of millions.
There have been health workforce projects in Kenya since 2009, but US funding for these types of programs has been dwindling. In my experience as a physician and health workforce expert, some of these funding cuts have greatly affected how we support health workers both at the national and the subnational levels.
Now that the Biden Administration is considering launching a new White House initiative for the global health workforce, they should make sure to focus on health systems, including the health workforce.
Funding cuts have greatly affected how we support health workers.
Here are seven areas of investment I hope the White House will focus their initiative on for stronger health system and better results.
These areas have been drastically cut and deemphasized. We need to establish more teaching hospitals and centers of excellence where health workers of all medical cadres are trained locally, at county and subcounty referral hospitals—not only in big cities.
And I don’t mean just doctors, nurses, and midwives. During COVID-19, we’ve seen the need for multidisciplinary specialist cadres to treat critically ill patients in ICUs and biomedical engineers to help maintain equipment in hospitals.
We have models in Africa like the College of Surgeons of East, Central and Southern Africa (COSECSA), for one, that can support this in rural areas and faculty exchanges can be scaled up. We need centers of excellence with state-of-the-art infrastructure and faculty so they can serve two purposes: provide high-quality services and train health workers at the local level without disrupting services.
We also need to work with medical training universities and colleges to ensure regular curricula review and to integrate quality improvement into health programs. Quality improvement must be part of national and subnational policies. Focal persons should be assigned to implement it at various levels of health care and ensure health workers can be trained and conditioned for implementation.
We need to teach health managers how to use data for informed decision-making. This includes helping them become better managers so they can respond to health workforce needs, mentorship and coaching so they can improve management, and systems that ensure real-time and up-to-date data to support decision-making. All of which call for a human resource information system with dashboards that can answer questions based on national and subnational needs, including the World Health Organization’s National Health Workforce Accounts, among other data required by health leaders for informed decision-making.
Another aspect of data for decision-making is supporting the implementation of, for example, the Workload Indicators of Staffing Need to allow countries to generate their own norms and standards for the health workforce and supporting productivity and labor market analysis and assessments. This can also be used to assess if a staff shortage is indeed a genuine shortage or artificially created.
We cannot provide high-quality services without a workforce that is motivated and has strong leaders.
Currently, most supervision is focused on specific programs and not on the workforce. But we are forgetting that we need to create an enabling environment for health workers, one that keeps managers focused on what needs to be done—not just programmatically but for the health workforce as well. Thus supervision needs to be prioritized and undertaken alongside program-specific supervision.
This is one that deserves a lot more attention. We’ve seen quite a bit of labor unrest among health workers in Kenya and South Africa, for example.
We need to engage employees so they better understand current human resources challenges and make sure their employers are aware of the issues health workers are facing so that together they can find ways to engage and come up with solutions. This calls for establishing and supporting regular employee-employer dialogue platforms such as work councils.
We have seen this increase during COVID, both at work and in the community, and it's gaining momentum, especially for the health workforce. Policies and guidelines need to be put in place to support workforce safety and wellness.
We need to support country and regional observatories for health workforce migration to monitor data on health workforce developments and mobility.
This is important because, for instance, Kenya was willing to have some of its nurses go and work in in Britain. But you ask yourself, who exactly is migrating? Are they solid managers who have years of experience? Or are these workers who have never been employed?
Observatories would help us understand what workers we are producing, who is unemployed, and who is available for migration, rather than consistently losing experienced workers who are needed at home to mentor the country’s younger health workers and provide high-quality services.
Are you paying health workers at government rates? If the pay is poor, how is that country also motivating the workers with non-financial incentives? What does the appraisal system look like? What's the work environment like for health workers?
These issues determine whether health workers are engaged or if they're absent—mentally or physically.
Sustainability is not possible without the right systems in place.
My parting shot: Sustainability is not possible without the right systems in place and stronger advocacy to ensure proper funding for health systems strengthening and mitigation of funding cuts to workforce investments.
We need projects at the country level that can dive deep on health systems strengthening, for instance to support government schemes of services for their health workers and appraisal systems that tie to productivity and data. A big global project is needed to synthesize what is happening at each country level and compile information to guide global leaders and thinking, as well as to scale up implementation and replicate good results between countries.
Get the latest updates from the blog and eNews




