Where We Work
See our interactive map

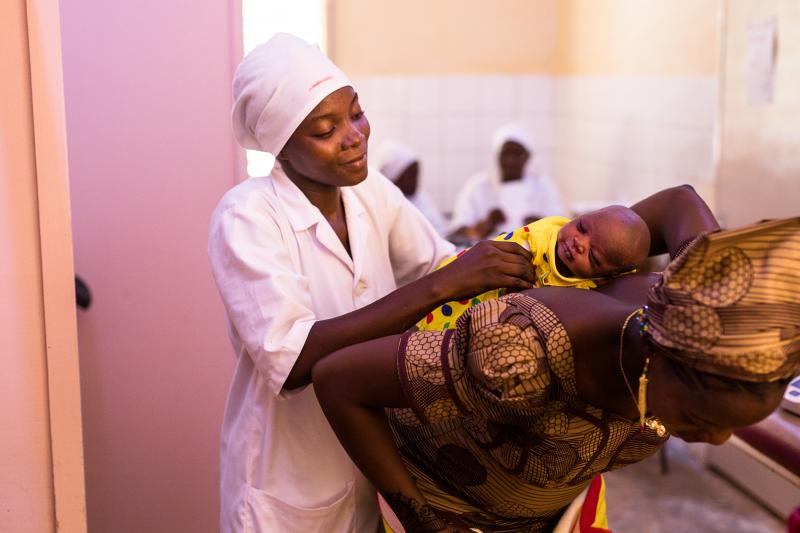
A health worker helps a mother and her baby at a health facility in Ouagadougou in 2017. Photo by Trevor Snapp for IntraHealth International.
Here's how our INSPiRE team in West Africa developed new indicators to monitor their progress toward more people-centered and efficient care.
Countries in West Africa have some of the highest maternal and infant mortality rates in the world. Women in this region face a 1 in 34 lifetime risk of maternal death and 34 of every 1,000 infants do not survive their first 28 days. An estimated 24% of women have an unmet need for family planning and only 1 in 5 women are accessing modern contraception.
Achieving universal health coverage—wherein all people have access to the health services they need, when and where they need them, without financial hardship—would turn these numbers around. One way to get there, the World Health Organization says, is through client-centered services integration. This is a way of providing a package of health services during a single visit—such as family planning and nutrition services and maternal care and newborn/infant care. And while it’s more efficient for the client and for the facility, it also means families who have to travel great distances to a health facility are more likely to get all the care they need.
This is a great way to advance universal health coverage in countries where access to care remains a big challenge.
It was in response to these challenges that IntraHealth introduced the INSPiRE initiative. Funded by the Bill and Melinda Gates Foundation, INSPiRE helps national governments in West Africa’s nine Ouagadougou Partnership countries integrate services for family planning, nutrition, and maternal, neonatal, and child health for women and their newborns. This way,
a mother who travels to the clinic for postnatal care with her newborn for a vaccination visit, for example, will also receive counseling about family planning and nutrition information, all in the same visit.“We have adopted the service integration approach which has enabled us to meet the needs of our clients, especially in terms of family planning,” says Nebenhide Gamba Ouedraogo, a midwife at the Urbain Health Center in Burkina Faso. “It has improved the quality of care and allows us to further reduce missed opportunities which, in turn, improves our indicators.”
Delivering services as an integrated package avoids missed opportunities to provide critical, lifesaving services for mothers and newborns. Through four points of entry—antenatal care, delivery, postnatal care, and newborn care—mothers can receive services they might not have otherwise received.“I really appreciated the fact that I came to weigh my child and the health worker took the opportunity to talk to me about family planning," says Felicia Kiboro, a client visiting the Niche Health Center in Burkina Faso for a well baby visit. "The health worker welcomes us. He takes good care of our children. He weighs them and gives us a lot of advice, especially on family planning. He also talks about COVID-19."
The INSPIRE model was introduced in 11 facilities across three flagship countries: Burkina Faso, Côte d’Ivoire, and Niger. After two years, the preliminary results in these facilities have been promising:
“Service providers are seeing remarkable progress in their center’s performance indicators thanks to improved family planning uptake and increased use of prenatal and postnatal services,” says Marguerite Ndour, INSPiRE’s project director. “This is a great way to advance universal health coverage in primary health care services in countries where access to care remains a big challenge and resources are limited to expand health structures.”
Measuring service integration is critical to monitoring progress but also to reinforcing provider behavior change in a sustainable way. In partnership with the Ministry of Health, INSPiRE helped develop indicators that measure service integration. This approach is a regional first, promising sustainable success.
In each country, composite indicators were developed for family planning, nutrition, and maternal, newborn, and child health. They were included in the national health information systems and in the facility-level data collection tools. At each visit, health workers are reminded to report on the services they delivered to their clients using data collection tools, which are then monitored at the district and the national level.
These new indicators provide useful data for decision-making as the integrated service model is implemented and scaled up nationally, but they also provide women and their families with sustainable access to a range of high-quality services that they haven’t had before.Get the latest updates from the blog and eNews




