Where We Work
See our interactive map

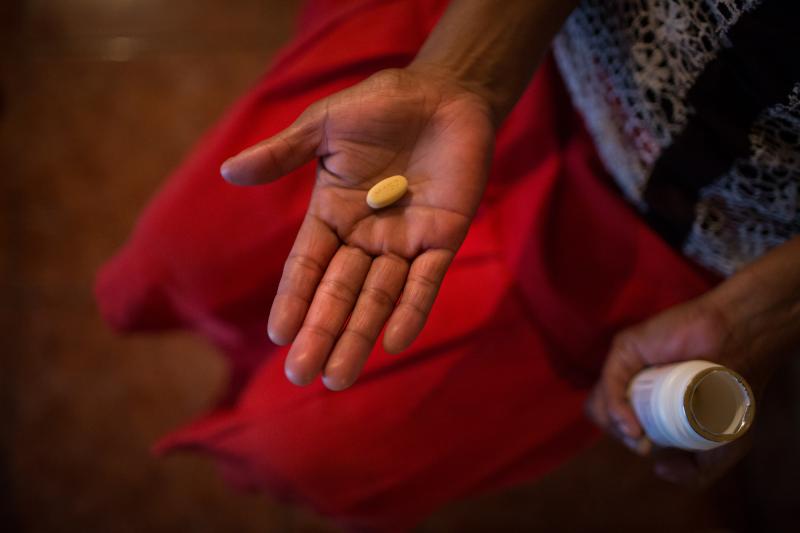
A client received HIV medication at their home in Guatemala in August, 2017. Photo by Anna Watts for IntraHealth International.
We’re adapting our health services to reach clients in new ways.
In Central America, the COVID-19 pandemic has created new barriers for people living with HIV to adhere to their antiretroviral therapy (ART) regimen. People living with HIV face lack of transportation, reduced clinic hours and sites, and fear of going to clinics—all of which make it harder for them to continue taking their medication.
So health workers from Nicaragua, El Salvador, Guatemala, Honduras, and Panama are using some new approaches to help their clients overcome these obstacles.
As part of the COVID-19 emergency response, many hospitals in Central America have reduced business hours, restricted access to outpatient consultation clinics and, in some cases—like at the Tela Hospital in Honduras—transferred HIV services to different clinics.
For clinic coordinator Dr. Nerlyn Gutierrez and his team, this was cause for concern. The health workers knew they needed to contact clients about the service location change, but had no way to communicate with them, which would make it hard for clients to obtain their medication or receive much-needed services.
So IntraHealth’s HIV Care and Treatment Project (HCTP) turned to the mobile phone platform alerTAR for a solution. The alerTAR system is a low-cost, CommCare-based tool that helps health workers at 26 ART clinics in El Salvador, Guatemala, Honduras, and Panama send treatment reminders via SMS to thousands of clients who may be cut off from their usual health facilities. Tela Hospital implemented the alerTAR system in 2019 to strengthen retention and prevent clients from abandoning their ART.
Using AlerTAR, José Gutiérrez, the data entry officer for HCTP, sent 394 clients text messages with important information about the new clinic location and daily reminders about appointments and medication intake. Thanks to the helpful messages, HCTP provided care to 389 people in the new clinic.
“Sending messages through alerTAR is an excellent way to keep patients motivated and show them that many people care about their health,” Gutiérrez says. “Patients who received the messages were very happy and grateful, since it’s difficult for them to attend their medical appointments due to mobility restrictions, economic limitations, and lack of public transport.”

alerTar training in Guatemala. Photo taken by Mario Fernando Hernández for IntraHealth International.
At the onset of the COVID-19 pandemic, fear of the virus became a barrier for some clients. Many stopped attending integral care clinics despite the facilities' protective measures, such as all staff using face masks, increased hand-washing, use of hand sanitizer, and physical distancing. Because of this, 149 of the HIV Care and Treatment Project clients were ready to abandon their treatment instead of visiting HIV clinics.
But we didn’t want to let that happen. With our partner organization in Nicaragua, the Nicaraguan Association of Positive People (ANICP + VIDA), we connected clients with their treatment.
ANICP + VIDA employs enhanced adherence counseling and helps people living with HIV recognize the importance of their treatment, identify barriers to adherence, and learn strategies to overcome them so they can achieve and maintain viral suppression. When they learned that almost 150 people were thinking about abandoning their HIV treatment, ANICP + VIDA pivoted—and processed patient authorizations to obtain the medicines their clients needed and deliver it to their homes. They organized a team, created geographic service routes, and leveraged transportation methods to provide an immediate and effective response.
The new approach worked. Between March and August 2020, ANICP + VIDA delivered medicines to 199 people and conducted 297 home visits in the Nicaraguan districts of Managua, León, and Chinandega.
"Thanks to the support of ANICP + VIDA, I can access my ART without risking a COVID-19 infection,” says Marcos, an HCTP client. “I feel very satisfied with the service and support."
Juanita*, 28, lives in Chiriquí, Panama, near the Costa Rican border. Each month she travels four to five hours, first by taxi then by bus, to visit an HIV clinic and pick up her ART medication. She has diligently kept up with her medical appointments and medicines despite the distance and her limited financial resources.
But when COVID-19 began to spread in Panama, she could no longer travel.
“I called Juanita to coordinate the delivery of her medication,” says Sayllin Martínez, an adherence promoter at David’s Integral Care Clinic. “She was worried about not taking her treatment.”
So Martínez went the extra mile, literally, to ensure Juanita and clients like her receive their medication during the COVID-19 pandemic.
“To deliver medication, each patient is visited at home and asked to submit and sign paperwork that allows us to pick up the medication at the David Clinic's Pharmacy,” Martínez says. “After obtaining the medicine, we return to each patient’s home to drop it off. In Juanita’s case, the process took me two hours and 50 minutes each way.”
IntraHealth International’s HIV Care and Treatment Project in El Salvador, Honduras, Panama, and Guatemala, is funded by USAID. It focuses on reaching clients with high-quality, stigma-free services and works together to enroll and retain as many people living with HIV as possible on treatment.
* Not her real name.
Get the latest updates from the blog and eNews




