Where We Work
See our interactive map


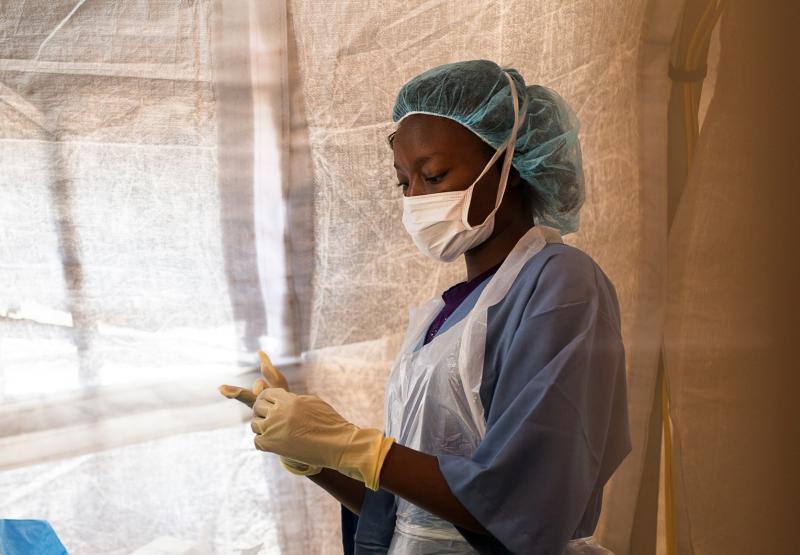
A health worker at an IntraHealth-supported mobile clinic in Shinyanga, Tanzania. Photo by Trevor Snapp for IntraHealth International.
Vaccine rollout, rising temps, decolonizing global health, and more.
COVID-19 stole the headlines in 2020—and revealed that most countries were vastly underprepared for a pandemic.
But it also shed light on incredible human ingenuity and fortitude. We saw frontline health workers navigate a deluge of COVID cases while also trying to keep crucial services available. We saw the fastest vaccine development in history. And we saw more clearly than ever our need for stronger supply chains, better mental health services, and new ways to fight misinformation.
These are just a few of the big global health issues that we at IntraHealth International will be watching and responding to in 2021. Read on for more.
While vaccines are already being deployed in the United States, the United Kingdom, Israel, and European Union nations, the rollout in other countries is lagging.
“The promise of equitable access is at serious risk,” said WHO Director-General Tedros Adhanom Ghebreyesus on January 18, 2021. “More than 39 million doses of the vaccine have now been administered in at least 49 higher-income countries. Just 25 doses have been given in one lowest-income country. Not 25 million; not 25 thousand; just 25.”
Vaccinating most of the global population may take years and millions of health workers. The WHO estimates that deploying vaccines to just 20% of global population will require about 1.1 million full-time-equivalent health workers.
Health workers must be at the front of the line for vaccine.
“Health workers must be at the front of the line for vaccines around the world,” says Andrew Brown, senior director of health workforce development at IntraHealth International. “So they can safely get on with the crucial business of providing it—along with other crucial health services—to their communities.”
So far, the COVAX Facility has secured around one billion doses for people living in the world’s 92 low- and middle-income countries. In 2021, vaccine producers will need to do more to quickly manufacture and provide affordable doses and national governments will need to address ”vaccine nationalism,” a mindset that is spurring countries to buy up many more doses than they actually need for their citizens, leaving other countries in the lurch.

The World Health Organization's #VaccinEquity campaign to ensure health workers around the world receive the vaccine. Graphic provided by the World Health Organization.
Vaccine nationalism is just the most recent in a long history of inequitable approaches to public health. And while many organizations and leaders are calling out racist and colonist ideologies dredged up by COVID-19, many others are calling for a complete overhaul of the colonialist approach to global health, pointing out that the system is and always has been set up to help colonizing countries thrive at the expense of others.
“We should consider who is defining international standards,” says IntraHealth’s Tembi Mugore. “These standards should reflect all countries, rather than just the wealthiest. The top-down, ‘do good’ model of development—where rich countries support poor countries— is outdated and needs to be transformed.”
This approach requires a complete change for most Western organizations, and one that reckons with racism as well. It’s no secret that America’s racism is at the root of most health inequities in the US, where Black mothers die during childbirth at a higher rate than white mothers, people of color are more affected by COVID-19 than white people, and Black men and women have lower average life expectancies than white men and women.
“Racism is a global system that affects all fields, including international development,” says Polly Dunford, president and CEO of IntraHealth. “US-based global health organizations like IntraHealth risk exporting our racism overseas with every flight we take and inflicting it on our partners and stakeholders—the very people we are meant to serve.”
It’s time for change. It’s time for global NGOs like ours to partner with local organizations and institutions to work for them—not the other way around. In 2021, we must start breaking down the very systems that built our organizations in the first place, including by rapidly preparing local organizations and governments to serve as the prime partners for development funding, including from the US Agency for International Development and US President’s Emergency Plan for AIDS Relief programming.
If ever a year highlighted the importance of health workers, it was 2020. Reports of their tremendous sacrifices saturated the news. Yet they still weren’t getting the supplies, support, and resources they needed to respond to the pandemic appropriately.
The World Health Organization designated 2021 the Year of the Health and Care Worker to highlight their important role during the pandemic but also encourage greater, ongoing investment in the global health workforce.
“In 2020 the world saw strikes by health workers in at least 84 countries, in many cases due to poor working conditions,” Dunford wrote in Devex. “If health workers’ needs are not met, our response to COVID-19—and any future pandemic—will fail.”
The WHO’s #ApplauseIsNotEnough campaign is calling for countries and donors to act in 2021 by investing in health workforces and making policy changes to support and protect them.
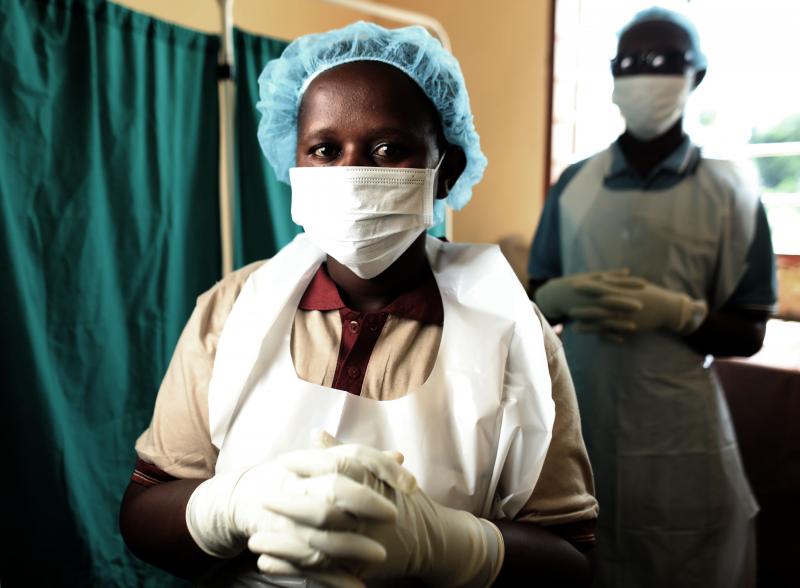
Health workers in Tanzania. Photo by Josh Estey for IntraHealth International.
When communities go on COVID lockdown, too many people lose access to the routines that keep them healthy. This includes HIV treatment, family planning and reproductive health services, maternal and newborn care, and services to treat and prevent noncommunicable diseases. Health workers have been working hard to keep those types of care available—and will continue to do so in 2021.
The WHO’s Pulse survey reported that almost every country (90%) experienced a disruption of health services to some extent. In some cases, health workers have been able to adapt services, like in Tanzania, where HIV services went mobile and new approaches helped keep HIV services available—even exceeding targets.
But there was also backsliding on past global health progress. In the last two decades, maternal deaths fell by more than 50% percent in 25 countries. But that statistic is likely to change because of COVID-related disruptions.
In 2021, we’ll be watching for greater investment and funding from the US and other major development in the health workforce, for COVID response and beyond.

A health worker in Guatemala uses CommCare, a digital health solution for outbreak response. Photo by Mario Fernando Hernández for IntraHealth International.
The World Meteorological Organization reported that 2020 was one of the hottest years on record during the hottest decade on record. Rising heat coupled with the extreme weather events and other disasters over the past 20 years have become more common and more costly and are pushing millions of people toward “an uninhabitable hell,” according to the United Nations.
The health workforce will be on the front lines of climate change.
The “Human Cost of Disasters” report recorded 7,348 major disaster events over the past 20 years that affected 4.2 billion people—including 1.23 million lives lost and $2.97 trillion in global economic losses.
Not only do these disasters affect food security and nutrition (earlier in 2020, the United Nations announced that 690 million people around the world did not have enough to eat—and the number continues to rise due to COVID-19), but regions with high food insecurity are also facing significant health challenges from preventable diseases. The health workforce will be on the front lines of climate change as demand for health services increases.
Now that the Biden administration has re-signed the Paris Climate Agreement and committed to achieving net zero emissions by 2050 alongside China and the European Union, there is a glimmer of hope but it’s not a short-term fix. We’ll be looking to new approaches, innovations, and national commitments in 2021.
Disease, political unrest and uncertainty, the trauma of natural disasters or violence, food insecurity—all weigh on us and affect our health, both mental and physical. And the COVID-19 lockdowns brought another stressor to the forefront—social isolation.
A study published by the Kaiser Family Foundation found that “53% of adults in the United States reported that their mental health has been negatively impacted due to worry and stress over the coronavirus.” And that is added to a health system that was already under-prepared to provide mental health services. Lancet reported that COVID-19 had a detrimental effect on people with depressive, anxiety, or obsessive-compulsive disorders in the Netherlands, and Devex highlighted the connection between depression, drug use, and a shortage of health workers.
For those not in social isolation, COVID-19 takes a different toll. Frontline health workers are overworked, understaffed, working without proper protection, and are experiencing overwhelmed intensive care units and skyrocketing death rates.
A recent review of health care professionals found a 23% prevalence of depression and anxiety, and 39% prevalence of insomnia during COVID-19. A recent International Council of Nurses report found that sixty percent of ICN national nursing associations received reports of mental health distress for nurses related to the COVID-19. In some cases, this has led to suicide. For others, it has led to burnout, depression, anxiety, and other stress-related illnesses.
This should be a wake-up call.
As COVID-19 spread in 2020, so did misinformation. Online, we saw bogus claims that masks were useless, that 5G cellphone towers were causing the disease, that it was all a hoax. When the vaccines were announced, there was talk that it would change your RNA, that it was actually a microchip implanted in your body to know your whereabouts, or that it would give you COVID-19 instead of preventing it.
Scientists and (most) leaders around the world tried to combat this misinfodemic by creating their own messaging campaigns. A group of scientists published the COVID-19 Vaccine Communication Handbook in early 2021 to respond directly to some of the more prevalent myths. And the WHO created a campaign to fight false COVID information on social media.
But it’s clear that public health agencies have less and less control over the spread of information, especially when it’s false. There have been some lessons learned but in 2021, health workers will be on the front lines of this battle against misinformation and its sometimes-deadly consequences.
Women leaders set records in 2020.
Countries with female leaders had lower COVID-19 death rates and better economic performance. Kamala Harris became the United States’ first female vice president and the first woman of color in the White House. And President Biden’s administration made history with the most diverse Cabinet in American history.
A century is too long to wait for gender equality.
A study in Proceedings of the National Academy of Sciences found that women’s health is better when women have stronger roles in their communities, especially when it comes to chronic diseases. But we have a long way to go, especially in the wake of COVID-19.
The pandemic has forced women to leave the workforce at much higher rates than men, as child care options disappeared and female-dominated fields were hit hard. The World Economic Forum’s Global Gender Gap Report 2020 reports that a 31.4% average gender gap still remains globally, and the largest gender gap is in political empowerment, which, if all trends continue normally, will close in about 100 years.
A century is too long to wait for gender equality in positions of power, especially when we know that women’s leadership leads to better women’s health.

Alice Boit is a nurse leader making sure her nurses are fully trained in Kenya. Photo by Patrick Meinhardt for IntraHealth International.
Most countries don’t include disability as part of their health agendas. And many services for the more than 1 billion people in the world who have disabilities are nonexistent or extremely underfunded. Health systems are leaving them behind, according to the London School of Hygiene & Tropical Medicine—even amid the Universal Health Coverage and Health4All campaigns.
“People with disability were more than twice as likely to report finding health care provider skills inadequate to meet their needs, four times more likely to report being treated badly, and nearly three times more likely to report being denied care,” the WHO reports.
The pandemic has exacerbated it all. Rehabilitative services and in-person education for children with different learning needs have been interrupted, opaque masks have made lipreading impossible. Persons with disabilities are often at higher risk of acquiring COVID-19, and information about the disease often doesn’t come in the necessary formats, such as Braille, large print, sign language, captions, audio, and graphics.
Health workers and national governments have a challenge ahead in correcting this and other service shortcomings for people with disabilities.
We can’t deny it—2020 changed us. Many of us switched to telemedicine, calling health workers over the phone or via video conferencing. Community health workers changed their local approaches, taking mobile services to their clients if they couldn’t get to a health facility. Preventive care and home care became more popular. Many of us simply went without care.
COVID-19 has changed the health workforce, too. As vaccines are rolled out in 2021, health workers will be called on to keep going, beyond the exhaustion, to be creative, to provide new services. We’re likely to see some bold new approaches and pioneering health entrepreneurship. In it, we’re likely to see glimpses of the future of health care—of the scenarios that might lead us to a more resilient future in global health.
Get the latest updates from the blog and eNews




