Where We Work
See our interactive map

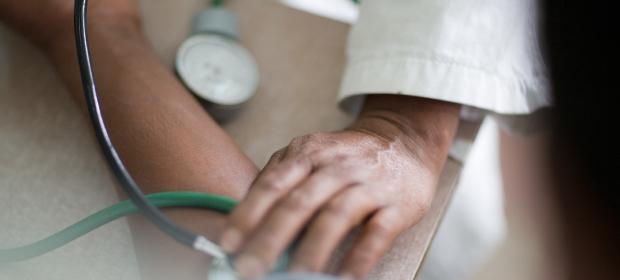
World Health Day 2013 is marked by a call for intensified efforts to prevent and control hypertension, also known as high blood pressure. The World Health Organization (WHO) estimates that worldwide, high blood pressure affects more than one in three adults aged 25 and over—or about one billion people—and is a major contributor to heart disease and stroke.
Altogether, hypertension is the world’s number one cause of premature death and disability.
For those of us who have an interest in the prevention of cardiovascular disease, this focus on high blood pressure, even for a day, is welcome indeed. High blood pressure is what we used to call a symptomless risk factor. Contrary to popular belief, people with high blood pressure do not know they have it unless they get tested and—worse yet—being tested once is not enough. Blood pressure has to be tested regularly, or it can become a silent killer.
Mulling this over was enough to get me into my time machine heading back to 1988. That year, a book was published by Faber and Faber called Prevention of Coronary Heart Disease and Stroke: a Workbook for Primary Care Teams, co-authored by me, along with Julian Tudor Hart and J.A. Muir Gray. The book is now out of print so you can’t run out to buy a copy, but I unearthed it today to remind myself of what we wrote.
Two major messages stood out and they still resonate in 2013. First, high blood pressure should be detected early and is both preventable and treatable through lifestyle changes. Second, a team approach to the detection and management of high blood pressure and other cardiovascular risk factors is essential if the burden of care is to be manageable.
In our book, we talked about the risk factors for heart disease and stroke, including high blood pressure. I wondered if the risk factors might have changed in the intervening years, but they haven’t; they are still lifestyle-based. It is what we eat, how much we exercise, and whether we smoke and drink alcohol to excess that affect the condition of our arteries and hearts.
We emphasized in our book that our clients were not likely to change their lifestyle behaviors simply because they were given a leaflet. There is a real art to effectively planning prevention and treatment with patients. And the key message we had was that this takes time—a luxury not always available to hard-pressed health workers.
We also wrote about the roles that nurses can play in primary care in detecting and managing hypertension, which at the time was pretty radical. Indeed, having a book jointly authored by a doctor and a nurse was unusual in itself back then. The reason for the joint authorship was to convince primary care teams that they should consider sharing the tasks involved in blood pressure control. Our clients needed time to discuss their fears and to hear messages about their health. They appreciated being able to talk to a knowledgeable health worker—not necessarily a physician—and there were some groundbreaking nurse-led programs implemented at that time.
About 25 years later, we are still talking about the same issues. How can health workers share tasks effectively and work as teams for the benefit of their clients?
In many countries where IntraHealth works, health workers have extraordinarily heavy workloads. Thinking about the effects of adding chronic disease prevention and control to their already overstretched clinics is the stuff of nightmares. To have any impact on the burden of chronic disease we need to explore new ways of working together wherein skills are used efficiently and people get the care they need.
Of course, the individual health care team is only part of the story. Public health measures are needed, too. In 1988, it was all about preventing smoking through high taxes on cigarettes and supporting people to give up the habit. Now it is about food and exercise, too.
Today, we know more and we have different tools. Social media has revolutionized the ways we communicate and its potential is still unrealized, especially in getting people to take notice of information. The primary care team needs to work with the larger public health team to get lifestyle messages out and ensure that they are seen and heard.
The new WHO global brief on hypertension (worth a read!) points out that detection and treatment demand a robust health system and a focus on all of the elements—good governance, money, buildings, equipment, information, and, of course, health workers. Detecting high blood pressure exemplifies exactly why health workers are central to health systems. With no health worker there is no one to operate and interpret the machine that measures blood pressure. Even with all the other elements in place, the system would be at a standstill without the health worker.
Tracking this silent killer won’t be easy. And without health workers, it won’t be possible at all.
Get the latest updates from the blog and eNews




