Where We Work
See our interactive map

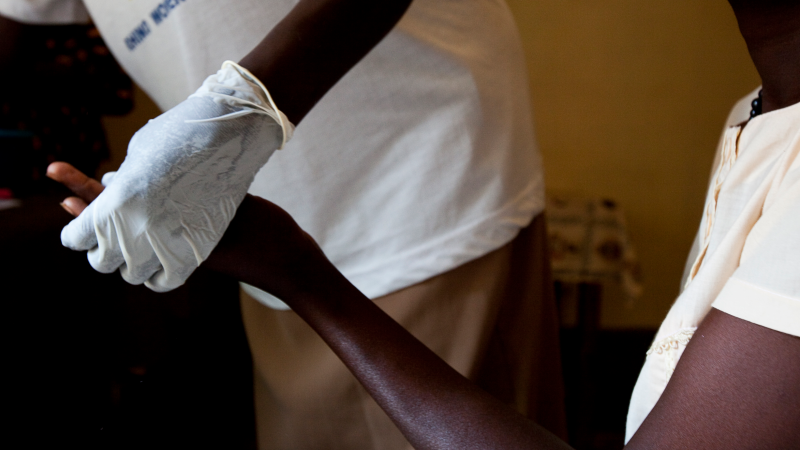
A nurse draws blood to test for HIV and begins counseling a client at the Saint Bakhita Health Centre in Yei, South Sudan. Photo taken by Trevor Snapp for IntraHealth International.
Violence, stigma, and other challenges I see every day as I provide HIV care to people in my community.
Every day, I go out into communities and talk with sex workers and their clients. I tell them about HIV and encourage them to get tested. And when I identify someone who is HIV-positive, I enroll them in antiretroviral treatment (ART), the drug regimen that will help them stay healthy and keep their viral load down, so they are less likely to transmit the disease.
I provide and connect the women to other services, such as family planning, screening and treatment for sexually transmitted infections, and services that respond to gender-based violence, which unfortunately many female sex workers in South Sudan face.
As a woman providing HIV/AIDS services in South Sudan, I’m proud of my work.
Here the HIV infection rate for the general population is 2.3%, but for female sex workers, it is 16%.
To reach the country’s goal of ending the HIV epidemic by 2030, we must connect those who are at high risk of contracting and spreading the virus with the right services. This includes identifying people who are HIV-positive (especially those who do not know their status), providing them with life-saving antiretroviral therapy, and helping them stay on their treatment. These steps will reduce AIDS-related deaths and prevent further transmission of the virus.But to do this, we must confront major challenges—and look to some proven solutions.
These women face stigma from the public and even from health workers, who often see them as spoiled and blame them for infecting others. This only increases the HIV infection rate in the country, and ultimately adds to the heavy workload for health workers. It leads female sex workers to hide, stop seeking treatment (12.1% of sex workers avoid care because of stigma or discrimination), or to self-transfer to another facility in search of friendlier services.
There is a shortage of health workers in the public sector in South Sudan. And the health workers who do still work in the sector are overworked, underpaid, and stressed. This creates low motivation to work. In the health field, we say practice makes work better, so if health workers lack the motivation to stay on top of their training, knowledge, and skills, the quality of work is compromised.
Low motivation among health workers also leads to high staff turnover in our public health facilities, as health workers often leave for better opportunities offered by nonprofits and other companies. When a health worker resigns from their post, it’s hard to quickly replace them, which can cause further staff shortages and interrupt HIV treatment for clients.
In my work to provide HIV services for female sex workers in areas where they cluster, I am often mistaken for a sex worker and male clients end up negotiating for sexual acts with me. This puts me at huge risk for gender-based violence.
Female sex workers face this danger every day. Almost half of the female sex workers we screened in 2021 as part of our community-based HIV services project—the USAID-funded Advancing HIV & AIDS Epidemic Control Activity—experienced a form of gender-based violence ranging from physical, emotional, and sexual to economical. Once we’ve identified this, we refer them to psychosocial support services and, if needed, we provide them with post-exposure prophylaxis.
The spread of COVID-19 has kept us from reaching female sex workers at times, which in turn has kept them from crucial services. Total lockdown and fear of exposure to COVID-19 hindered access to HIV treatment, as public transportation was not allowed to operate. We shared information with communities, made personal protective equipment (hand washing facilities, hand sanitizers, face masks, etc.) available at hotspots, and limited the number of clients to groups of 5-10 at a time for services to limit congestion per ministry guidelines.
IntraHealth’s Advancing HIV & AIDS Epidemic Control Activity is the only PEPFAR-supported project focused on providing community-based ART to female sex workers in South Sudan. This method is not only working to increase the number of HIV-positive people on treatment, but it is also improving retention of clients on care and increasing the effectiveness and efficiency of the country’s efforts toward HIV epidemic control.
To date, 1,238 HIV-positive female sex workers are on ART in Juba County.
The Advancing HIV & AIDS Epidemic Control Activity is training frontline health workers to provide services in their communities that are free of stigma and discrimination to everyone, regardless of who you are and what you do. Those who test positive for HIV are initiated on treatment at the community level and monitored for good treatment outcomes. This increases demand for and access to health care services.
Good supervision improves health worker skills and services and provides opportunities for feedback. I imagine with better supervision and management, more health workers will be retained and we will not have to constantly rebuild relationships in the community to keep people on ART and sustain HIV prevention. Good supervision can help eliminate our biases and keep us at our best while serving our communities.
As a woman providing HIV/AIDS services in South Sudan, I’m proud of my work. Female sex workers respect, trust, and gain confidence when working with women health workers. I, and other health workers AHEC has trained, listen to them. They feel comfortable sharing their social and sexual issues with us and that creates a bond—one that can lead to healthier futures.
The Advancing HIV & AIDS Epidemic Control Activity in South Sudan is funded by the US Agency for International Development.
Get the latest updates from the blog and eNews




