Where We Work
See our interactive map

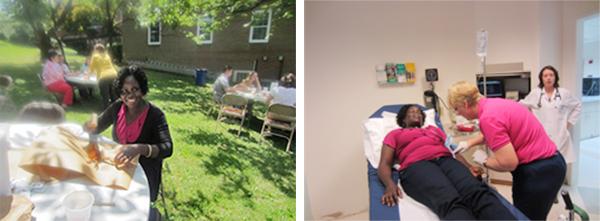
This post originally appeared on the CapacityPlus blog.Even though I ended up in the hospital on my trip to the US, I was glad I tried the local cuisine. I had flown from my home country of Kenya into Baltimore, Maryland, to meet with my colleagues at IMA World Health. I thoroughly enjoyed an IMA staff picnic (where I tried crabmeat for the first time) and will cherish the fun I had with my coworkers—with most of whom I had only worked with virtually. About two hours after the picnic, my tongue was swelling. I thought that I had bitten it, but couldn’t recall doing so. I went into a panic and called my colleague for help. We raced to the nearest health facility (a hospital), where I was quickly attended to.After being at the waiting bay for about ten minutes, I started having difficulty breathing. The nurse at the reception immediately informed the emergency nurse and I was quickly shown to one of the observation rooms. A doctor and another nurse came in to give me oxygen for my breathing and a strong intravenous antihistamine to arrest the allergic reaction. I was monitored for about 30 minutes, then transferred to another hospital by ambulance. On arrival, I was received by a nurse who confirmed the referral and immediately took me to one of the observation rooms where a medical officer took down the history of my allergic reaction and monitored my symptoms. I didn’t realize until that hospital visit how much people in Maryland love crabmeat. One nurse stopped short when I told her what caused the allergic reaction. “You mean you can’t have crab anymore?” she exclaimed. “I would take Benadryl with me everywhere just to eat my crab!”
Sub-Saharan Africa bears 25% of the global disease burden yet only has 3% of the world’s health workforce.
As I stabilized and began to breathe normally, a lot went through my mind. I reflected on the many rural health facilities that I have visited in Africa, as part of my work with the IntraHealth International-led CapacityPlus project. For the first time I truly understood what the global health worker crisis means and how critical it is to have the right numbers of skilled and motivated health workers on hand where they’re needed. The WHO statistics on the health worker shortage, particularly in sub-Saharan Africa where I live, appeared in bold text in my mind. Sub-Saharan Africa bears 25% of the global disease burden yet only has 3% of the world’s health workforce. In total I was cared for by 14 heath workers within about five hours in the two health facilities that I visited: two records officers; two nurses at the triage; four more nurses coming in at different times; two medical officers at different times, each with a nurse to take notes on their instructions; and two paramedics in the ambulance. I pictured a rural health facility in northern Kenya I had visited that’s working to attract and retain at least one full-time medical doctor to care for the population there that is in need of equally good health care.I left the hospital feeling very lucky to have received the urgent care services I needed. My situation could have turned tragic if I had delayed or had not had access to a properly staffed health facility. And I keep thinking about the many lives that have been lost in places where the kinds of services and skilled health workers I had access to were not available.
Get the latest updates from the blog and eNews




