Where We Work
See our interactive map


Health workers are key, says Kayinamura Mwali Assumpta, along with ensuring they have the training, support, and equipment they need.
We’re almost at the halfway mark for meeting the Sustainable Development Goals, including dramatically reducing maternal mortality, ending preventable newborn and child deaths, and ensuring universal access to sexual and reproductive health services. But new reports show that many countries are off track.
I sat down with Kayinamura Mwali Assumpta, a pediatrician who serves as IntraHealth International's deputy chief of party and technical director for our USAID-funded Ingobyi Activity in Rwanda. We talked about her work and research to improve maternal and child health in Rwanda, including helping health workers scale up evidence-based practices, and what she thinks needs to happen next.
During my medical school internship in the pediatric department, I had very good mentors. And what moved me is the way you can see a baby coming in very sick and then when you give them the right treatment, in a few days—or even a few hours—the baby will start to smile and to play. It's a personal satisfaction to see the progress of a baby in a very short time.
After finishing my master’s degree in pediatrics, I led the neonatal service in CHUK, the teaching hospital in Kigali. A colleague working with the Ministry of Health saw my work and asked me to help pilot the first neonatal unit in a rural district hospital, in Rwamagana. That was around 2009, and at that time only teaching and referral hospitals could admit babies.
So we planned, designed the program, developed neonatal protocols, trained health workers, and started a small unit. Then we published the results. The ministry's head of maternal and child health was very happy and asked me to lead the scale-up. Now all the district hospitals have at least a Level 2 Neonatal Unit.
Through my work I saw how newborns are linked to mothers—you can't achieve good newborn health outcomes if you’re not also working on maternal health. So that's why I started also focusing on maternal health, and began working at nongovernmental organizations implementing maternal and child health projects.

Dr. Assumpta Kayinamura Mwali helped pilot the first district neonatal unit in Rwanda at Rwamaganda District Hospital. Photo by Innocent Ishimwe for IntraHealth International.
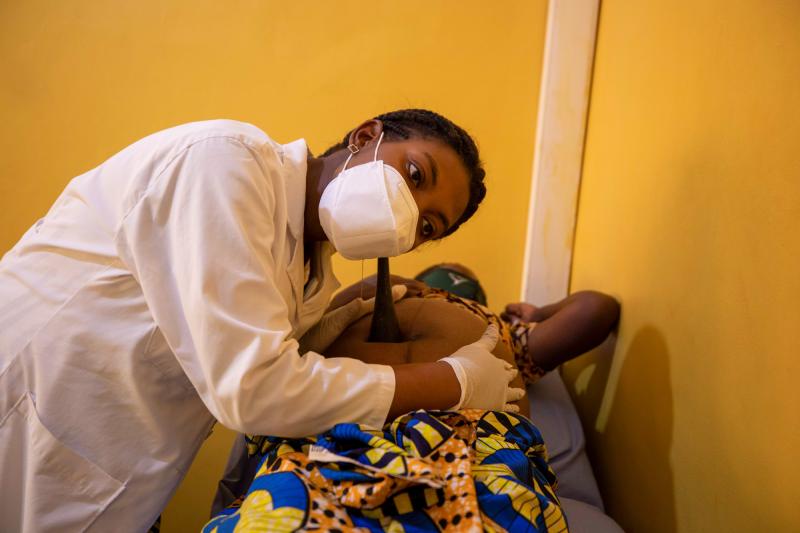
Janviere Bamushima, a maternity nurse, examines a pregnant woman in Ngoma District. Photo by Innocent Ishimwe for IntraHealth International.
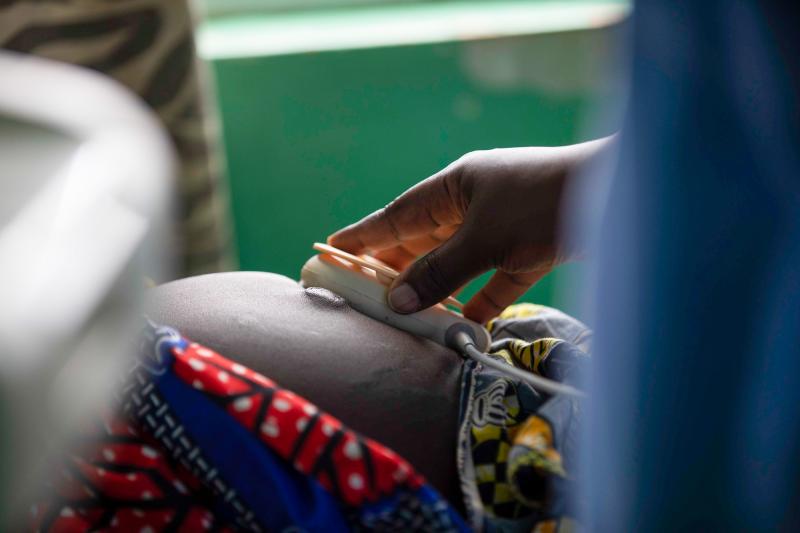
A health worker examines a pregnant woman in the maternity waiting room at Kibungo Referral Hospital. Photo by Innocent Ishimwe for IntraHealth International.
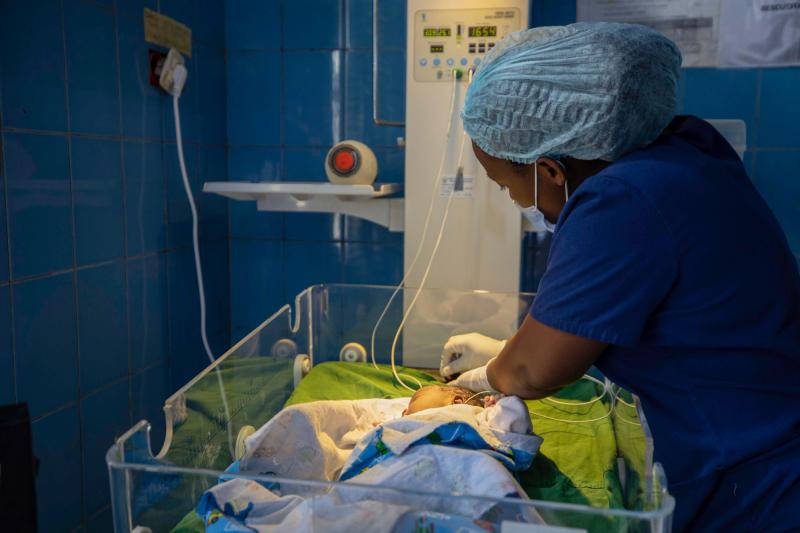
Nurse Cecile Mutuyimana cares for a newborn in an incubator at Kibungo Referral Hospital. Photo by Innocent Ishimwe for IntraHealth International.

Uwimana Jeanne, a health worker, poses outside of Nyanza District Hospital. Photo by Innocent Ishimwe for IntraHealth International.
Rwanda is implementing all the high-impact maternal and child health interventions, from antenatal care to childbirth up to adolescent care, but we still have some problems with the quality of care. First, the shortage of staff in maternity, pediatrics, and in health centers and primary health care is a big challenge. When the workload is too high, health workers become stressed and of course this affects their motivation and the quality of care they provide.
Another problem is the lack of sufficient equipment, like CPAP (continuous positive airway pressure) machines, ultrasound machines, incubators, etc. We have basic equipment, but not enough, and it is not well maintained due to the lack of spare parts in the country.
The Ingobyi Activity uses training and clinical mentorship to build the capacity of health workers and improve maternal and newborn care. Last year we designed a neonatal nurse mentorship program with over 25 mentors and 80 neonatal nurses in district hospitals, to improve the use of neonatal equipment, infection prevention and control, and family-centered care. For example, a recent study in Rwanda revealed that respiratory distress syndrome was contributing to most preterm deaths, but pediatricians were not using CPAP machines to save babies. So mentors trained neonatal nurse specialists on those machines. Now neonatal nurses in the district hospital are using that equipment. Overall we’ve seen improvement in health outcomes–neonatal mortality has reduced.
Through the USAID-funded MOMENTUM Safe Surgery in Family Planning and Obstetrics project we are leading a learning agenda on the active follow-up of pregnant women who have already had a cesarean delivery, to prevent them from having an emergency c-section. We know that an emergency c-section increases the risk of complications, such as risk of uterine rupture. So we are identifying these women in antenatal care, and immediately referring them to nurses at health centers to follow up and make sure they reach the hospital and receive a delivery plan. So this helps ensure they have an elective c-section, instead of waiting until they have signs of labor to come to the hospital. With this intervention, we are already seeing almost a 50% reduction in emergency c-sections.
Ingobyi conducted research on compliance and utilization of the right package of antenatal care. We found that, although ANC coverage has improved in Rwanda, provision of the recommended ANC package is inconsistent—health workers are not screening many women for malnutrition or syphilis or testing them for anemia. We also identified challenges health workers were facing, like stockouts of blood collection tubes. And with these data, we advocated to the Ministry of Health to avail those kits and reagents. We are beginning to see improvements in the delivery of the recommended package of ANC services.
Countries and donors need to invest more in health workers, including community health workers (CHWs), and in the supplies they need. Because if we have enough skilled, motivated, and equipped health worker teams, we'll save and improve more moms’ and babies’ lives.
For example, Rwanda is investing in reforming its community health workforce. Previously we had two kinds of CHWS—the ASM (Agents de Santé Maternelle), all female, in charge of maternal and newborn health, and binomes (female-male teams) in charge of integrated community case management of childhood illness, family planning, and nutrition. Now the country is training all CHWs to deliver a comprehensive package of all community health services (14 modules) to their assigned households in the villages.
CHWs are contributing a lot to improving maternal and child health. So countries should provide comprehensive training for CHWs and ensure they have the equipment they need to do their work. Ingobyi recently piloted an eLearning course for CHWs to replace the current didactic refresher training. Results show it was effective in increasing CHWs’ knowledge, including in community-based newborn health management.
Additional research is also needed, because when we have local evidence and use it to address gaps, we see big changes. In Rwanda, we have a program on maternal and perinatal death surveillance and response, and through confidential enquiry into maternal death survey, we can see the root cause of those deaths, and take appropriate measures to prevent them in future.
Meet Assumpta at the International Maternal Newborn and Child Health Conference, taking place May 8 - 11 in Cape Town, South Africa! She’ll present IntraHealth’s research and work in Rwanda during two sessions:
Get the latest updates from the blog and eNews




