Where We Work
See our interactive map


A baby is measured for size at the Busowobi Health Center in Iganga District, Uganda. Photo by Tommy Trenchard for IntraHealth International.
This hospital is making changes to reduce preterm births—and they're paying off.
When 25-year-old Aida Adongo started bleeding during her seventh month of pregnancy, she knew she had to seek care quickly. By the time she reached the Lwala Hospital, the nearest health facility in her community, she had already delivered one twin. The other was born safely at the hospital, thanks to the swift response of the medical team when she arrived.
In Uganda, preterm births—babies born before 37 weeks—like Aida’s are likely to occur for women who do not attend antenatal visits. This often means women living in rural areas, far from health facilities, are at a higher risk of having their babies early. Approximately 226,000 babies are born too soon every year in Uganda and of these, 12,500 children under five die due to preterm complications.
The Ministry of Health in Uganda is committed to improving the survival and health of newborns through high-quality maternal and newborn care, especially for babies who have a low birth weight or are sick.
Lwala Hospital in the Kalaki District of eastern Uganda is one of the health facilities IntraHealth International’s USAID-funded Regional Health Integration to Enhance Services in Eastern Uganda (RHITES-E) project supports.
Through essential newborn care mentorships, RHITES-E helps the Lwala Hospital and others like it maintain functional neonatal units and maternity wards staffed by skilled midwives.“We struggled to deliver high-quality care for our babies born too soon and small,” says Clere Amunyo, the health worker in charge at the Maternity Lwala Hospital.
“However, with support from RHITES-E, we now have a fully functioning neonatal unit.”RHITES-E supplies the maternity unit with basic obstetric equipment, including delivery kits, caesarean kits, penguin suckers (to clear a baby’s mouth and nose), and manual resuscitators. RHITES-E has also helped the Kalaki District review over 90% of the perinatal deaths (a dramatic increase from 5% in 2018), which helps health workers understand and tackle the root causes of perinatal deaths and implement collective actions to prevent them. Since the training, there have been no perinatal deaths.
My hope was restored when I received good care from the midwives here. My babies are strong and I am happy.
The midwives at the maternity ward have also been trained on kangaroo mother care, an effective method of holding a baby that involves skin-to-skin contact and reduces mortality for hospitalized infants with low birth weight by 40%.
This is how Aida’s preterm twins survived.
“I lost my first twins at six months,” Aida says. “I worried this would happen again. My hope was restored when I received good care from the midwives here. My babies are strong and I am happy.”
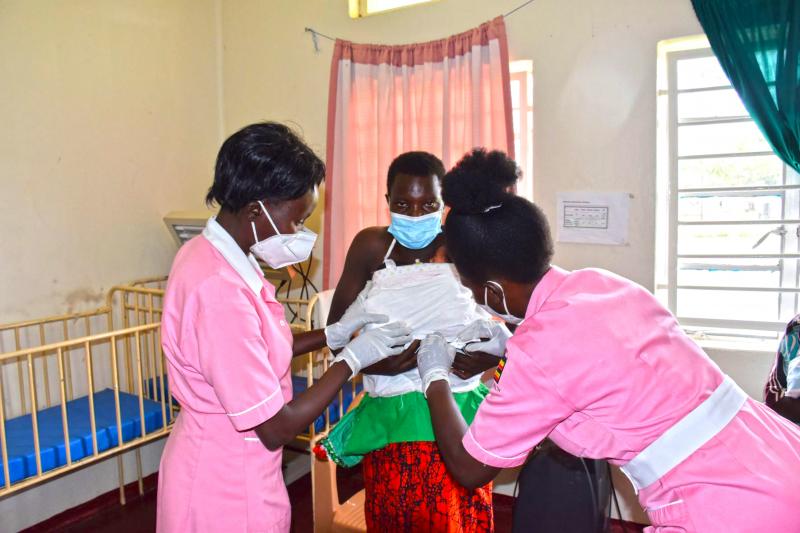
Health workers help Aida with kangaroo mother care at the health facility.

Aida with her newborn twins.
RHITES-E is training more midwives through onsite mentorship and coaching to implement kangaroo mother care and to make sure preterm babies aren’t separated from their mothers, which has proven to be effective in nurturing the newborn while providing care and treatment for the mother at the same time.
But the hospital’s leadership has changed more than just their approach to medical treatment. They are also tackling community-driven factors that lead to preterm babies by working with local leaders to address teenage pregnancies—the leading cause of preterm babies at hospitals—through health education and life skills workshops. The teenage pregnancy rate in Uganda is 25% and is highest in the Teso region, which is home to Kalaki District, at 31%. And school closures to due to COVID-19 have only increased early pregnancy rates for young women.
“We conduct intentional community engagement activities to create awareness around teen pregnancies,” says Ruth Enyimu, the senior hospital administrator. “We work collectively to empower the girls and their families on prevention measures.”
The hospital staff offer health education and counseling sessions to adolescents and young women based on the “Four Toos” (too early, too soon, too many, and too frequent) concept that addresses the dangers of early pregnancy and how it can be avoided.
Amid these successes, the hospital still struggles with an inadequate ambulance referral system; a dilapidated infrastructure for maternal, neonatal, and child health; and insufficient equipment for optimal service delivery. However, with the help from a government results-based financing grant (funding that is only released once a project has achieved specific results) for 51 districts to improve reproductive, maternal, and child health, hospitals are making progress. For example, now the hospital can transport emergency cases thanks to this type of government funding.
For now, the hospital is working to make sure every baby born prematurely receives high-quality care. And it’s working—more little beings are surviving.
Get the latest updates from the blog and eNews




