Where We Work
See our interactive map

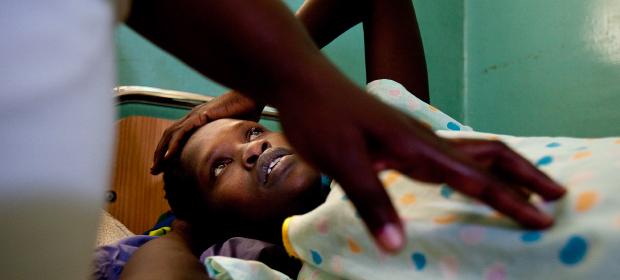
“Bring technology to me, not to a low-resource setting,” said Stembile “Tembi” Mugore, a trained nurse and midwife from Zimbabwe, at IntraHealth’s recent SwitchPoint 2013, challenging the audience to question their own assumptions about how and why they innovate.
It was one of the most tweeted quotes of the event, and it reminded me why our mission at IntraHealth focuses on health workers rather than a specific disease or approach: Medical advances and health technology breakthroughs will not save lives if we don’t also invest in the people delivering them.
I recently had the pleasure of sitting down with Mugore to talk about her career, her chosen field of midwifery, and the promise and pitfalls of introducing new technologies into midwifery practice in Africa.
When Mugore was growing up, she dreamed of becoming a nurse. At the time, in 1974, the educational opportunities for advanced nursing in Zimbabwe were limited, so she left to seek training abroad. She completed nursing school in Scotland and began her career as a nurse in London.
She loved nursing, but knew the clinical areas she found most interesting—advanced liver and renal disease and intensive cardiac care—would not be in high demand in Zimbabwe, where she hoped to return one day.
Mugore had enjoyed her six-week obstetrics rotation during her nursing program, and knew that midwives were in high demand back home, so she pursued additional training to become one.
And she loved it. Mugore worked and thrived in the United Kingdom as a midwife. She found nothing more rewarding than seeing a couple through the entire antenatal care process and finally sending them home with a healthy baby.
A natural teacher and mentor, Mugore immediately grasped that the midwife’s role extends beyond clinical care. When asked about a client who stands out, she remembers a 15-year old girl in labor who came into the maternity hospital, scared and completely unprepared for what to expect. Mugore said she had to act equal parts the professional and ‘big sister.’ This young mother needed someone to empathize with her, reassure her, and explain things in a compassionate and calm way. Mugore needed to build her trust and care for her emotional needs as well as her physical ones.
Having a rapport with her clients made Mugore happy—and a better midwife.
In 1984, Mugore had the opportunity to return to Zimbabwe to teach nursing and practice as a midwife in her home country, and she jumped at the chance.
Mugore knew that working conditions would be more challenging in her home country, but she hadn’t realized that the difference would strip her job of what she found most rewarding—communicating with clients, building trust, and utilizing all of her skills to provide the high quality care she was trained to give.
In Zimbabwe, she found the practice of midwifery characterized by constant improvisation and stress. She couldn’t consistently provide the best care, and there simply wasn’t the time or supportive environment to build relationships with clients. So Mugore focused on teaching, finding a job training in-service providers and incorporating family planning into pre-service nursing education.
Eventually an opportunity emerged to work as a training advisor with IntraHealth (known then as INTRAH). Her first major assignment brought her to Uganda which was just emerging from years of civil war. The health sector was starting to rebuild, and the Ministry of Health wanted to roll out training for nurses and midwives in family planning, reproductive health, and eventually safe motherhood.
In the UK, Mugore had learned best practices in midwifery care, but in Uganda, Mugore learned most of what she knows about “extraordinary midwifery”—how to handle cases when things go wrong. It’s also where she met Anne Otto—a midwife who inspires her to this day. Otto had a calm, empathetic approach in the most challenging circumstances, when most professionals would panic. She inspired everyone around her to focus on the mother and the baby, to focus on what they could do and not on things they couldn’t control.
It was in a rural health center in Uganda where Mugore saw a mother suffering from a post-partum hemorrhage so severe that, to this day, she can’t erase the image of all that blood. She talks with admiration of the two midwives who sprang into action and saved the mother using nothing other than their “guts, skills, and hands.”
The world has made a lot of progress in making pregnancy and childbirth safer since then. In the last 20 years alone, the number of women dying from pregnancy and childbirth complications has been cut in half. But Mugore doesn’t think this is enough.
More than 800 women still die every day from causes related to pregnancy and childbirth—and too many midwives around the world go to work to deliver too many babies with too few supplies and too little training and support.
Mugore says the “elusive Millennium Development Goal Number Five” cannot be reached without addressing these every day challenges.
Mugore is excited about technology and its potential for mitigating some of these challenges.
She’s most excited about communication tools like simple SMS text messaging; professional isolation is a huge barrier to providing quality care, and connecting midwives to other midwives and their supervisors, and to sources of information and support, is essential.
Mugore is also enthusiastic about new medical technologies. But, she warns, technologists must be careful not to miss the point: There is a tendency to think of technology as its own end, as if the technology alone will save lives. It’s great if the tools are designed to work in humid settings, operate with low bandwidth, or recharge using solar energy—but first and foremost technologists should design tools for the health workers expected to use them.
Mugore reflects on a recent exchange she read on a community of practice listserv. Someone was seeking a suitable test-location for a portable ultrasound device designed for low resource settings. Many midwives on the listserv balked, pointing to the need for very basic supplies, not a fancy ultrasound machine. From her own practice as a midwife, Mugore knows the value such a device brings: It can help a midwife make quick and accurate decisions about care. But the request didn’t mention the benefits to midwives.
The technology itself is not misguided, she says, it’s the approach.
Don’t make a device for a low-resource setting and test it on me. Make it for me.
When asked about the theme of the International Day of the Midwife, The World Needs Midwives Now More Than Ever, Mugore smiled and said, “Of course we need more midwives in more numbers, but it’s not just numbers. Midwives need skills and supplies and ongoing support from the health systems in which they work. We are far from using the skills of existing midwives optimally to address issues of maternal and neonatal mortality and morbidity. Midwives need the world now more than ever.”
Get the latest updates from the blog and eNews




