Where We Work
See our interactive map

Sub-Saharan African populations and economies are growing at unprecedented speed with a population growth of 2.7% annually and economic growth of 4.4% annually.
Africa has the fastest-growing middle class in the world, with 313 million people (roughly the population of the US), 34% of Africa’s population. This growing middle class is demanding higher-quality and more specialized medical care from both the public and the private sector.
Despite having the worlds’ largest disease burden, Africa has the lowest ratio of health workers per population.
At the same time, all African countries have committed to providing universal health care to their populations, which will require a dramatic expansion in the provision of health services. Yet a number of bottlenecks are making this difficult to achieve.
Africa, despite having the worlds’ largest disease burden, has the lowest ratio of health workers per population. In recent work that IntraHealth International conducted with the World Health Organization, we calculated that the global shortage of health workers, which is largest in Africa, will expand from 12 million to 18 million by 2030, with a 6 million shortage in Africa. With the fastest-growing population in the world and some of the worst high school graduation rates, Africa will be challenged to train enough health workers to meet needs.
In addition, health needs are changing from that of infectious diseases and maternal and child health to a new agenda of chronic and noncommunicable diseases, such as high blood pressure, diabetes, and cancer.
These new conditions will need different types of health workers, including specialty nurses and physicians. In addition, such care is more technology-heavy and requires talented operators to use the equipment and interpret the results and biotechnicians to maintain and repair the technology.
In fact, as aging increases demand for health care in developed countries, increasing these regions’ reliance on foreign-trained health workers, Sub-Saharan Africa will need to train even more health workers just to meet its own needs.
There are solutions.
One such solution is to find the intersection of public and private health systems, leveraging the existing and ready infrastructure, technology, workforce, and experience that comes from such deeply rooted organizations with local presence. In Kenya, for example, IntraHealth, GE Healthcare, and USAID are partnering to ensure that Kenya has enough health workers to meet its needs.
IntraHealth and partners have launched a loan program for health professional students so that more students can enter school. Its coordination with the government ensures that loans will be repaid.IntraHealth will also rely on its deep relationship with health professional councils to ensure that the new types of health care workers are legally recognized and integrated into the health systems. IntraHealth will continue to work to strengthen professional councils and regulators so that they can properly oversee a rapidly growing private sector.
IntraHealth has designed a social impact bond (a form of development investment designed to bring a new set of investors into the emerging markets) that will enable for-profit investors to invest in preventing dropouts from health professional schools. (IntraHealth’s work has revealed that up to 60 percent of health professional students in many countries drop out between enrollment and graduation.)
And IntraHealth is also starting to provide human resource management services, such as health worker recruitment, staffing, management, and training, directly to the private sector to increase its efficiency.
IntraHealth, GE Healthcare, and USAID are partnering to ensure that Kenya has enough health workers.
Just this week, the Ministry of Health of Kenya and GE Healthcare marked another step in the development of sustainable health care, with the inauguration of a $13 million skills and education facility for health care professionals. GE Healthcare committed to training 10,000 health professionals, including biomedical technicians, laboratory technicians, x-ray technicians, and other health workers.
The center will pull from GE’s decades of experience supporting health systems around the world—the existing and ready experience I referred to above.
It’s also innovative in its model. As part of the program, GE is not just selling equipment to the Government of Kenya, but rather it is surrounding leased equipment with a long-term system of service and training. That’s purchasing integrated solutions for results, rather than purchasing a box. The novel system and its new types of health workers will be integrated with Kenya’s licensing and regulatory system to ensure sustainability.
Naturally, this new approach will require learning on all sides, as all new ideas do. Governments must improve their ability to govern the private sector, to design good contracts, and to properly monitor the fulfillment of these contracts. The private sector must improve its understanding of governments’ values, goals, structure, and processes
.If these public and private parties join together in this way, all of the African people can potentially benefit.
This post originally appeared on The Pulse, a health, science, and technology publication by GE Healthcare.
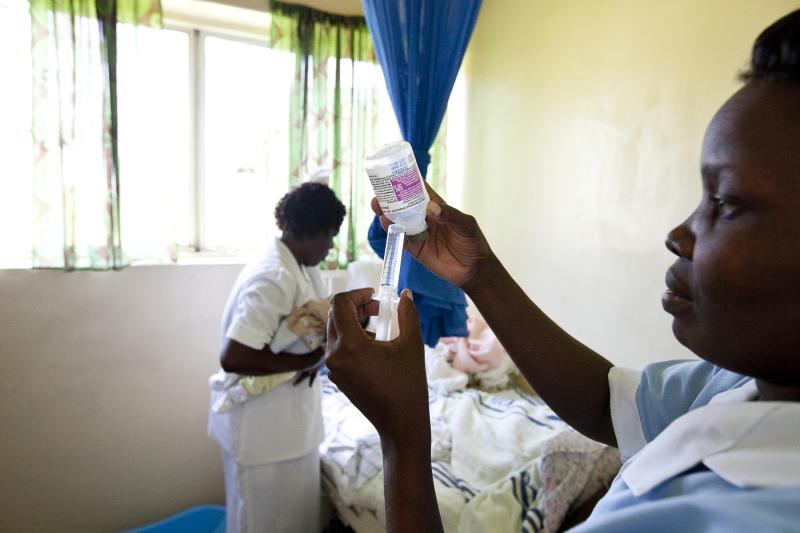
Photo by Trevor Snapp for IntraHealth International.
Get the latest updates from the blog and eNews




