Where We Work
See our interactive map

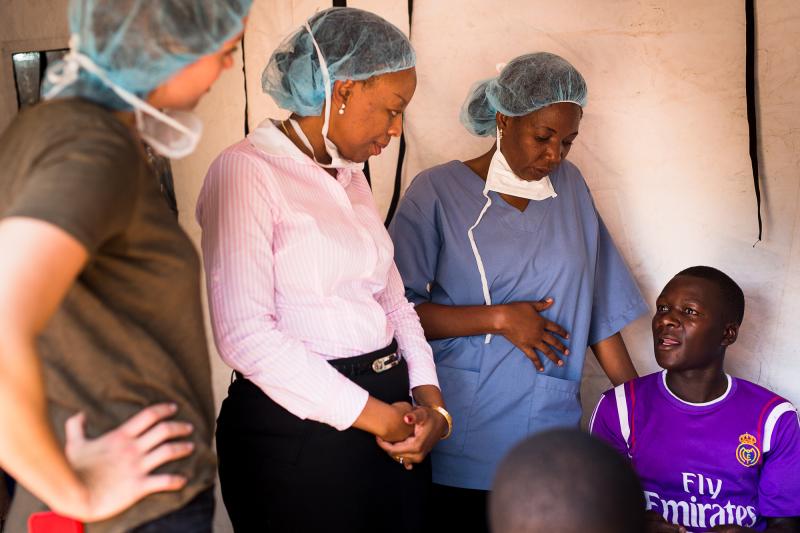
Lucy Mphuru (center left) talks with health workers and clients at an IntraHealth-supported mobile clinic in Shinyanga that provides voluntary male circumcision services. Photo by Trevor Snapp for IntraHealth International.
Three questions with Lucy Mphuru, leader of IntraHealth’s work in Tanzania.
Lucy Mphuru has a big job.
Every day, she and her team at IntraHealth International in Tanzania work with frontline health workers and government partners to improve health services in a country of 58 million—1.6 million of whom live with HIV.
In 2018, there were 72,000 new HIV infections in Tanzania, and 24,000 people died from AIDS-related causes. The country has a way to go toward its 90-90-90 goals—gender inequality and stigma against people who live with HIV make this work much tougher.
But Mphuru and her team are getting results.
This year alone, they’ve reached over 450,000 men.
In the seven lake regions, they’ve partnered with the Government of Tanzania to provide voluntary medical male circumcision services (VMMC), which lower men’s risk of acquiring HIV through heterosexual sex by around 60%. Since 2016, they’ve boosted VMMC access and uptake by over 200% and decreased the cost per client by nearly 40%.
This year alone, they’ve reached over 450,000 men with VMMC services.
Mphuru sat down with us to answer three questions about how her team is shaping the future of HIV care in Tanzania—locally and sustainably.
For any program to be sustainable, you must have a strong relationship with the government. We do, and that has helped us a lot.
Our team developed a stakeholder-involvement model that ensures the government—from the national level to the community level—is involved in everything we do, from planning to implementation to monitoring and evaluation. We orient them on all our activities from the beginning, do joint programming to scale up solutions together, and often get ideas from them that we would never have thought of.
This is a great example of country ownership. And it’s more sustainable.
For example, at one point, we were thinking of hiring retirees or interns to help carry out our VMMC efforts—we would have had to train them and pay them, but we weren’t sure where else to find the additional staff to do it, because health worker shortages are still a challenge in many regions.
But during our conversations with the government, they suggested instead using a reasonable number of their own health workers from regions that have already reached VMMC saturation—these were health workers who were already trained on VMMC and who wouldn’t be leaving their own clients without care by stepping away temporarily.
Now the government regularly allocates their own health workers for temporarily VMMC work, even in regions our project isn’t directly supporting.
This is a great example of country ownership. And it’s more sustainable, because they’re not relying on our staff to provide these services. The model of this approach could be used in most understaffed regions to get stronger results like these in a shorter time.
Watch: Empowering the Health Workforce in Africa | Interview with Lucy Mphuru
The government had often complained that the information in implementers’ databases never matched their own health management information system, the national DHIS2 database.
This is a problem, because you need your HIV services data to be accurate, complete, and up-to-date if you want to make fast, informed decisions based on them—where to allocate additional resources such as health workers, for example, or where there are gaps.
But it happens because some NGOs use their own data-collection tools to collect their own project performance data, which they then enter it into their own databases for reporting to their donors. And then separately the same information is captured using the government tools and reported through the government channels into the national DHIS2 database.
We do things differently when we gather our data.
As a result, there are discrepancies in the service delivery and uptake data, the data quality varies, and it isn’t always timely. And besides those problems, relying on NGO staff to supply and enter data just isn’t sustainable for the country.
So we do things differently. We work directly within the existing government structures to gather our data. This includes training and working alongside the government health workers—mentoring them on how to correctly capture data on a daily basis, how to clean them up, and how to do monthly reporting using the government tools and database.
And we work with the health management focal person in each district to make sure the data that goes into the national DHIS2 is high-quality and timely. Then we extract those data from the national DHIS2 whenever we need to report on them.
So now, any time you pull VMMC data from the IntraHealth database, it never differs from the national database.
By working this way, we’re not only strengthening HIV services in Tanzania, we’re also strengthening the government and its ability to manage data and maintain a strong health system.
Most of the time, when you walk into a health facility, you’ll find plenty of women, but no men. So I’m most excited about the opportunities we have to engage men in the health care delivery system.
This is a group that is not easy to access, if you’re talking about health-seeking behaviors. But because so much of our HIV-prevention work in Tanzania focuses on VMMC, that gives us an opportunity.
This year alone, we’ve reached more than 450,000 men with VMMC services, including testing services for 60% of them (around 270,300). Now imagine we could integrate other health services into all these visits.
We already do this for some services, such as screening for tuberculosis and sexually transmitted infections, and adolescent sexual health. But we could do much more—services related to nutrition, gender-based violence, family planning, screening for hypertension and diabetes, hepatitis B vaccinations, counseling on harmful alcohol use, healthy diet and exercise, and more.
In January, we’ll start integrating more services into our VMMC offerings. We really want to take advantage of this opportunity to more proactively engage men.
This piece is part of IntraHealth's celebration of 40 years of commitment to health workers. Follow along: #TheFutureOf #IntraHealth40 #HealthWorkersCount
Lucy Mphuru is IntraHealth International’s country director in Tanzania and director of the Tohara Plus Project.
Watch: Testimony from the Front Line | Lucy Mphuru at SwitchPoint




