Where We Work
See our interactive map

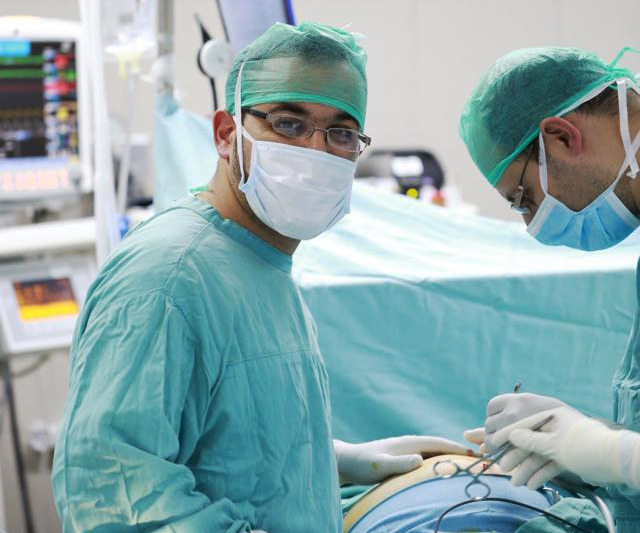
A surgeon at work in the West Bank, where USAID-supported NGOs have been forced to cease their activities. Photo courtesy of IntraHealth International.
IntraHealth International’s Palestinian Health Capacity Project shut down its activities on January 31—eight months before the project was scheduled to end—due to a request by the US Agency for International Development (USAID) in response to the new Anti-Terrorism Clarification Act.
This early termination will affect more than 120,000 clients who seek specialized medical care outside the West Bank and thousands of West Bank health workers who had been benefiting from the project’s preservice and continuing education and digital health improvements.
Since 2013, IntraHealth led this five-year, USAID-funded project that strengthened the West Bank’s health system by reforming its patient medical referral system and better preparing its health workforce to meet the population’s diverse needs. But in December, USAID asked IntraHealth and other USAID-supported NGOs in the West Bank and Gaza to end projects by January 31, due to the new act.
The quality and availability of health care will suffer today for Palestinian patients.
The project was on track to meet its objectives, but without its final eight months to transition its interventions to the local health sector, the sustainability of the program’s results is at risk.
“The years the project has invested in creating more self-reliant and stronger health systems, supported by the American people, are at risk of being wasted,” says Pape Gaye, president and CEO of IntraHealth. “The quality and availability of health services will suffer today for more than a hundred thousand Palestinian patients. We will also lose the opportunity to learn from and document the unique experiences of strengthening health systems in an area prone to conflict—lessons that could inform some of the biggest development challenges we face around the world today.”
The West Bank has very few tertiary-level hospitals that can provide advanced medical care and access to specialists is limited. When clients need specialized care that’s not available in the public health system, the Palestinian Ministry of Health refers them to local private- or NGO-managed hospitals or to hospitals abroad. Referrals drastically increased in recent years—from 8,000 in 2000 to 62,000 in 2013—and nearly half were directed to service providers outside the West Bank, mostly in Israel.
Referrals are also expensive—in 2014, the annual cost of referrals peaked at $100 million.
But the Palestinian Health Capacity Project helped reform the referral system, defining referral eligibility protocols, standardizing referral approvals and processing, and negotiating agreements with referral hospitals on better prices for certain medical services. The project developed an eReferral web-based application to track and regulate referrals and minimize delays in much-needed care. The project also helped set up customer service centers where clients could ask questions and process paperwork.
The improvements and yearly savings will be jeopardized or lost.
These efforts led to dramatic improvements in the overall appropriateness of referrals (referrals following new eligibility protocols rose from 41% to 88% in 2016) and helped reduce the total cost of referrals from West Bank health facilities to Israeli hospitals by 34%, or about $32.6 million annually. They also streamlined the process for both clients and hospital administrators.
Ceasing the project’s activities now—without a transition plan implemented—will affect 122,000 Palestinian clients who receive referrals for medical treatment outside the Palestinian public health care system. The improvements through referral reform and yearly savings of 120 million NIS ($30 million) will be jeopardized or lost.
The Palestinian Health Capacity Project improved health worker preservice education, continuing professional development programs, and licensing and certification systems.
The project equipped Palestinian nursing educators and students to better care for clients with complex medical needs by introducing a new competency-based critical care nursing curriculum at all nursing colleges in the West Bank. And it integrated patient safety and service quality principles into undergraduate health sciences programs, revised residency program curricula to match international standards, and established guidelines for continuing professional development for health workers.
The critical care nursing curriculum will face difficulties in sustainability and compliance.
Terminating the integration of safety and quality principles into undergraduate health sciences programs alone will affect 1,500 undergraduate health professional students currently enrolled. Losing the improvements in residency curricula will affect 500 residents currently enrolled in the four residency programs. And the critical care nursing curriculum, without the oversight and monitoring the project provided, will face difficulties in sustainability and compliance by college administrations, affecting the 600 undergraduate nursing students who are currently using it.
The project also improved the governance and use of the national health information system (HIS) to expand access to health information and increase accountability and efficiency of health facilities and workers.
By working to integrate the HIS with other systems and build the capacity of stakeholders at the national and facility levels to lead HIS initiatives and use data to inform health-sector decisions, the project helped the Palestinian Ministry of Health save 427,000 NIS ($122,120) by independently implementing its HIS in Tubas Turkish Hospital.
The project’s early end jeopardizes about 2.1 million client records in the HIS. It also inhibits the development of a continuing professional development electronic system intended for use by all health professional associations in the West Bank—this affects 100,000 health professionals. Once fully implemented, the system would have provided access to information and online courses, and would have allowed providers, for the first time, to track health education, enhancing the capacity to plan for health professional development and providing a mechanism for licensing and relicensing for health workers.
This forced early closure blocks to the road to self-reliance in the West Bank.
The project invested more than $2.2 million in developing digital health information systems and tools for referrals and continuing professional development, as well as a business intelligence tool, all of which have enhanced the quality of health care and increased timely access to information for decision-making and planning. While many aspects of the system have been installed, the full cycle of its work has not been tested yet, and the project’s closure will negatively affect its successful administration and sustainability.
“IntraHealth is proud to have worked on locally tailored and innovative solutions to address the largest barriers to sustainable access to essential health services in the West Bank, including addressing the high number of patients who must seek services in Israel or in private Palestinian or NGO-managed facilities,” says Salwa Bitar, IntraHealth’s chief of party for the project. “The forced early closure on such short notice prevents the effective transition of these solutions and blocks the road to self-reliance in the West Bank.”



