Where We Work
See our interactive map

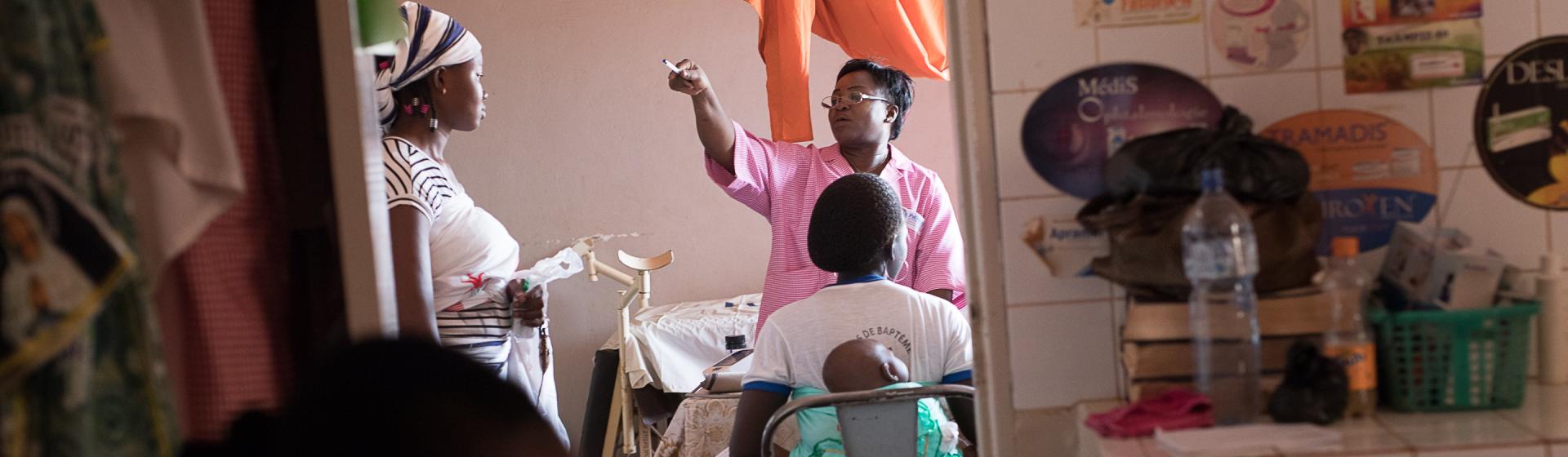
What will it take to build the ideal health workforce?
There are 7.6 billion of us on the planet today.
That’s 7.6 billion working adults, infants in diapers, nursing mothers, teens planning their futures, elderly people, and many, many more. We each have different hopes and requirements. And our health care needs change dramatically over the course of our lives.
So how do we provide health care for everyone?
If we have a prayer of achieving universal health coverage, it has to start with health workers. These are the pros on the front lines of health care, the lab techs and scientists behind the scenes, the advocates and funders and policy-makers guiding the big picture. Without all of them, health care simply doesn’t happen.
But we’re facing some big challenges when it comes to our global health workforce. There’s a shortage of health workers, for one thing—it could reach 18 million by 2030, according to the World Health Organization, unless we manage to create 40 million new health sector jobs before then.
Fortunately, more countries are beginning to focus on their health workforces as a sustainable investment for their populations’ future health and prosperity.
So, what will it take to build the ideal health workforce of the future? Here are seven issues that are likely to shape the field:
There is no #MeToo campaign for women health workers around the world—but there should be. There would be plenty to say.
Despite the fact that women make up the vast majority of the world’s health workforce, they occupy relatively few top spots. And they face rampant sexual harassment, discrimination, and even assault throughout their careers.
An assessment of sexual harassment in Uganda’s health sector, for example, found it to be rife with quid pro quo sexual harassment.
“Supervisors may use performance appraisals to settle scores for refusing sex, or may favor those who submit to demands for sexual favors,” writes Constance Newman of IntraHealth International. The consequences for a woman’s career can be enormous—including punitive transfers, demotions, and much more.
Ugandan women aren’t alone. Women health workers around the world experience similar barriers. But as we shed more light on these problems and more women rise to leadership roles in the health sector, health workplaces will demand greater equality, and more health workers will be able to focus their full professional time and energy on their patients.
Slapping. Kicking. Pushing. Verbal abuse. These are just some of the types of everyday violence health workers face around the world. In some US states, nursing is considered to be more dangerous than being a police officer or a prison guard.
Routine violence is enough to chip away at the quality of care anyone could provide, to say nothing of the emotional toll it takes on health workers.
And then there are the more devastating attacks. The war crimes wherein ambulances are looted, hospitals bombed, patients killed in their beds or sent fleeing into the streets. A 2017 report by the Safeguarding Health in Conflict Coalition found that the extent and intensity of violence against health workers globally remained alarmingly high in 2016, and that there is little to no accountability for those who commit them.
This can’t continue. The health workforce needs protection, support, and safe, decent working conditions in order to offer effective care for all, whether it’s during peacetime or in a warzone.
So often, we hear seasoned professionals tell students and youth organizations: “You have the power to change the future.” But that’s not the whole truth.
The fact is that today’s massive generation of young people—half the world right now is under 30—will change the future, whether they want to or not.
This is why we need to make more room for young workers, both in the frontline health workforce and in the field of global health. The millions of bright new candidates entering the workforce every year need roles they can sink their teeth into, mentoring without condescension, and the room and training to lead the way.
In the minutes you spend reading this article, new study results, tools, ideas, and breakthroughs about human health and disease are pouring into the health care field. And health workers face the challenge of keeping up with the flood.
But high-quality education is prohibitively expensive for many aspiring health workers. Even after graduating from nursing school, for example, there’s the ongoing costs and time involved in updating your training on a regular basis. Can you get away from work? Who will cover for you? Will you have to pay out-of-pocket and take time away from your family responsibilities? Is it worth the bother and expense?
Of course it is—lives depend on a health worker’s level of knowledge and expertise. But it’s not easy.
Many experts are looking to eLearning as the magic solution to affordable, accessible education. It’s relatively cheap to roll out, after all, and convenient for students who need flexibility. But quality often varies, and even the leading course-design companies are still grappling with how to balance the cost effectiveness of one-size-fits-all courses with the targeted, contextualized, and often hands-on training health workers need.
Another solution is to provide affordable financing for students who want to become health workers, but can’t afford school. Kenya, for instance, has introduced the Afya Elimu Fund, which provides low-interest loans for health professional students in Kenya. So far, 2,478 fund recipients have graduated and 62% of those employed are already paying back their loans.
More creative solutions like this could help prepare more aspiring and existing health workers with the training they need.
More countries than ever are making decisions about their health workforces based on solid data.
In 2013, for example, Namibia became the first country to assess its every public health facility to find out exactly how many and what types of health workers each facility needs to meet the health care demands of the communities they serve. As a result, the Ministry of Health and Social Services has changed various policies and procedures, and now uses those data to make decisions for planning and deploying its health workers.
And every day, countries are digitizing more of their old paper-based personnel files, using software such as the open source iHRIS to help manage their health workforce information.
Data will only become more important in the years to come, as more countries rely less on international aid and take ownership of their health sectors. Solid evidence will help funds stretch further, and bring universal health coverage within reach.
Other types of technologies will play a key role for the health workforce of the future, too. Apps that aid in frontline health care, communication systems that help health workers report potential outbreaks and stop them before they start. Whatever the technology, it doesn’t have to be flashy—it just has to work within contexts of the people using them.
If we want to make true, sustainable improvements to global health, we have to look beyond health care. As human beings, our experiences outside of the clinic—our education, personal finances, employment, gender roles, and so much more—all play their own parts in shaping our individual health and well-being.
“If you wake up in the morning and think ‘How am I going to get through this day?’ because you don’t have $1.50 to feed yourself or your family, then you’re not going to be thinking first about health care,” says Pape Gaye, president and CEO of IntraHealth International. “If we want to transform health, we have to look at more than just health care.”
We’re likely to see more smart, creative partnerships toward this end in the future, both among nonprofits and private-sector organizations and among health workers who team up, for instance, with factory owners who want to offer their employees HIV services, or with motorcycle taxi drivers who can spread health-related messages to their clients.
None of us knows what new disease, or environmental disaster, or medical breakthrough will affect global health in the decades to come. We’re making headway in investing in health workers, yes—but setbacks are frequent, and the future is uncertain.
The health workers of the future will face all this uncertainty and more—and so will we all. Investing in the systems that offer them training, support, and safe work environments is something we can do for them today.
This post was originally published by Global Health Writes.
In Dublin, Ireland, in November 2017, the health workforce of the future was at the heart of discussions among 1,000+ health workforce experts and global health specialists from around the world, at the Fourth Global Forum on Human Resources for Health.




